Understanding Postpartum Bleeding and Knowing When to Seek Help

Partner Support Tips That Make Postpartum Recovery Smoother
November 7, 2025Safe Skin and Hair Treatments You Can Begin After Your Postpartum Check‑up
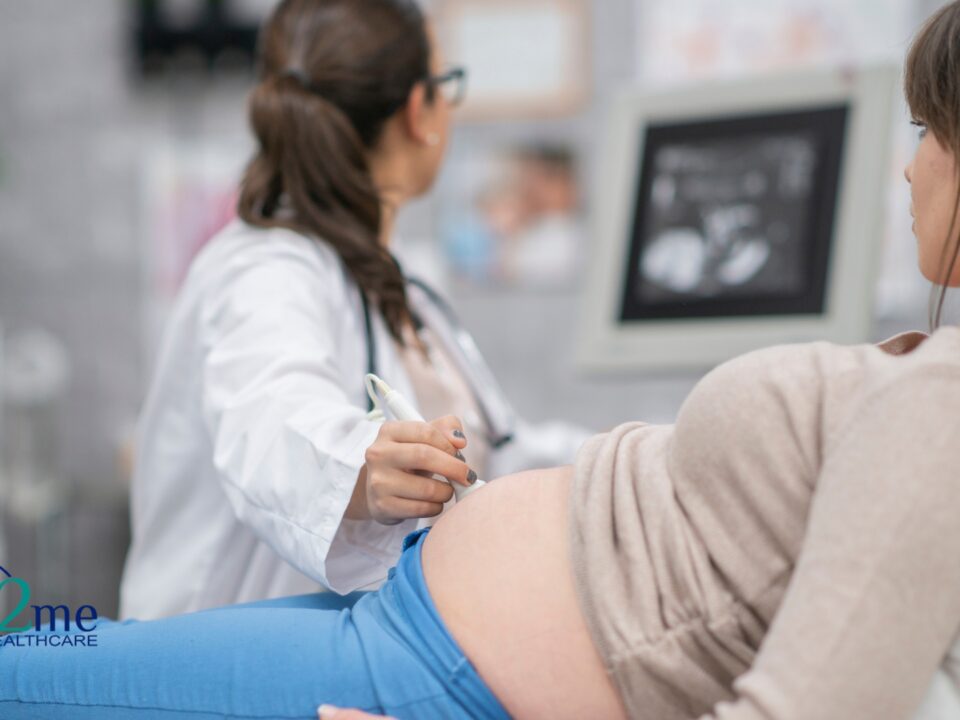
December 19, 2025The journey into motherhood is a transformative experience, but recovery after childbirth brings its own set of challenges and natural biological processes. postpartum hemorrhage (PPH)One of the most common and often concerning aspects of postpartum recovery is vaginal bleeding, medically known as lochia.
This process is a normal and necessary function of the body as it heals, yet distinguishing between a healthy recovery and a dangerous complication, like postpartum hemorrhage (PPH), is crucial for maternal health and safety.
Understanding Postpartum Bleeding
Postpartum bleeding, or lochia, is your body shedding the uterine lining after delivery. It normally lasts four to six weeks and follows three stages:
- Lochia Rubra (Days 1–4): Heavy, bright red flow with small clots (under golf ball size).
- Lochia Serosa (Days 4–10): Lighter, pinkish-brown, and watery.
- Lochia Alba (Weeks 2–6+): Light, white, or yellow spotting that eventually stops.
Increased bleeding during activity or breastfeeding is normal, and it signals you need rest. Always use pads, never tampons.
When to Seek Help Immediately
While postpartum bleeding is normal, it’s important to be aware of the signs that the bleeding is abnormal or that an infection is developing. These signs, often subtle at first, can escalate quickly and require immediate medical intervention.
The most serious complication is Postpartum Hemorrhage (PPH), which is the excessive blood loss that occurs within 24 hours (primary PPH) or up to 12 weeks after delivery (secondary/late PPH). It’s a life-threatening emergency.
Signs of Postpartum Hemorrhage (PPH)
Call your healthcare provider or emergency services immediately if you experience very heavy flow, such as soaking through one or more maxi pads in an hour or two, which is a clear sign of excessive bleeding, or if you’re passing blood clots that are bigger than a golf ball.
Another concerning symptom is bleeding that suddenly returns to heavy, bright-red flow after it has already lightened, as well as feeling dizzy, lightheaded, or fainting, which indicates a sharp drop in blood pressure due to blood loss.
Finally, if you have an abnormally fast or irregular heart rate (tachycardia), as that’s your heart attempting to pump enough blood through your body, or if you’re feeling pale, cold, or clammy, or experiencing sudden shortness of breath or extreme, uncharacteristic weakness.
Signs of Postpartum Infection
A postpartum infection, such as endometritis, can occur when bacteria enter the reproductive tract. While often treatable, it needs prompt attention. Contact your healthcare provider right away if you notice foul-smelling discharge, fever, or chills. You should also contact your healthcare provider if you experience severe pain or tenderness in the lower abdomen or pelvis that is not related to normal cramping and isn’t relieved by pain medication.
Factors Affecting Recovery and Risk
While every woman experiences some bleeding after childbirth, certain factors can increase the risk of postpartum hemorrhage (PPH) or other complications. Understanding these can help you recognize your own potential risks and seek prompt care when needed.
PPH is often explained using the “4 Ts,” which describe its main causes:
1. Tone (Uterine Atony)
This is the most common cause of PPH. After birth, the uterus must contract firmly to compress the blood vessels where the placenta was attached. When it fails to contract effectively, it is called uterine atony. The uterus feels soft or “boggy,” and bleeding can become excessive.
2. Trauma
This refers to physical injuries sustained during delivery, such as tears to the cervix, vagina, or perineum. Sometimes, bleeding can also come from hidden hematomas, pockets of blood that collect internally and may not be immediately visible.
3. Tissue (Retained Placenta)
If pieces of the placenta or its membranes remain inside the uterus, they can prevent it from contracting properly. This retained tissue often leads to ongoing bleeding and requires medical removal.
4. Thrombin (Clotting Disorders)
Clotting problems, either pre-existing or acquired during pregnancy, can prevent the blood from clotting normally. These conditions, known as coagulopathies, make it difficult for the body to stop bleeding naturally.
Your likelihood of developing PPH may increase if you have a history of PPH, have experienced a prolonged or difficult labor, have had an operative or cesarean delivery, or have other underlying risk factors.
Because your cervix and reproductive system continue to heal and adjust in the weeks after birth, follow-up care such as postpartum cervical screening, including your Pap smear after childbirth, is also an important part of ensuring your recovery progresses safely.
Self-Care and Prevention
Managing postpartum bleeding is also about managing your recovery process. Simple self-care measures can help your body heal efficiently. The most important rule is to limit activity, especially in the first two weeks. Excessive movement can increase bleeding. If you notice a bright red gush of blood, it’s a sign you need to sit down and rest.
Do not use tampons, menstrual cups, or douches until your healthcare provider gives clearance, usually at your six-week check-up. Inserting anything into the vagina can introduce bacteria and lead to infection.
Keep track of how many pads you use daily and the size of any clots you pass. This information is vital for your healthcare provider if you need to call them with a concern. Lastly, proper hydration and a diet rich in iron can help your body recover from blood loss.
Prioritizing Your Postpartum Health with OB2Me
Understanding the difference between normal postpartum bleeding (lochia) and a serious issue is vital to your recovery. Never dismiss warning signs like soaking pads quickly or passing large clots; your instincts are your most valuable tool. Prompt attention to any red flags, be it excessive bleeding or signs of infection, ensures a safe and complete transition into motherhood.
For personalized guidance and round-the-clock peace of mind during this critical fourth trimester, OB2Me offers direct, reliable access to certified nurse midwives. Trust your body, recognize the signs, and use OB2Me to navigate your postpartum journey with confidence.