Understanding Velamentous Cord Insertion

Understanding Postpartum Contraception and Fertility Recovery
February 20, 2026
The Complete Handbook for a Calm, Low-Intervention Birth
March 20, 2026The umbilical cord is the literal lifeline between a mother and her developing baby. In a typical pregnancy, this cord attaches firmly to the center of the placenta and is protected by a thick, rubbery substance that ensures blood and nutrients flow without interruption. However, in approximately 1% of singleton pregnancies, a variation occurs known as velamentous cord insertion (VCI).
While the name sounds complex, it describes a specific anatomical difference in how the umbilical vessels connect to the placenta. For many parents, a VCI diagnosis can feel overwhelming.
The Anatomy of the Umbilical Cord
To understand VCI, it is helpful to first understand a regular insertion. Usually, the three blood vessels of the umbilical cord are encased in Wharton’s jelly, a gelatinous tissue that prevents the vessels from kinking or being compressed as the baby moves. These vessels travel directly into the mass of the placenta.
In velamentous cord insertion, the umbilical cord does not reach the placenta itself. Instead, it attaches to the fetal membranes, which is the thin sac surrounding the baby. The blood vessels must then travel through those membranes, while unprotected by Wharton’s jelly, until they eventually reach the placenta.
Because these vessels are essentially naked as they traverse the membranes, they are significantly more fragile. They lack the structural armor provided by the jelly, making them susceptible to being pinched, compressed, or even torn.
Why Does It Happen?
The exact cause of VCI isn’t fully understood, but the leading theory is a process called trophotropism. As the placenta grows, it tends to migrate toward the areas of the uterus with the best blood supply. If the umbilical cord stays fixed in its original spot while the placenta moves away, the cord ends up tethered to the membranes by these trailing vessels.
Risk Factors
While VCI can happen in any pregnancy, research has identified several factors that increase the likelihood. VCI is found in up to 15% of twin pregnancies, especially those where babies share a placenta. There is a higher correlation between VCI and pregnancies achieved through IVF. If the placenta is located low in the uterus, the risk of VCI increases. Finally, babies born with only two vessels in the cord instead of three are at higher risk for VCI.
Potential Risks and Complications
The primary risk of VCI stems from the lack of protective Wharton’s jelly around the umbilical vessels. Without this cushioning, the baby may face intrauterine growth restriction (IUGR) if nutrient delivery becomes inefficient. Furthermore, fetal movement can cause vessel compression, leading to heart rate dips.
The most critical complication is vasa previa, occurring in 6% of VCI cases. Here, unprotected vessels traverse the cervix, and if these rupture during labor or when water breaks, it leads to rapid fetal blood loss. Fortunately, with early ultrasound detection and a planned C-section, survival rates exceed 95%.
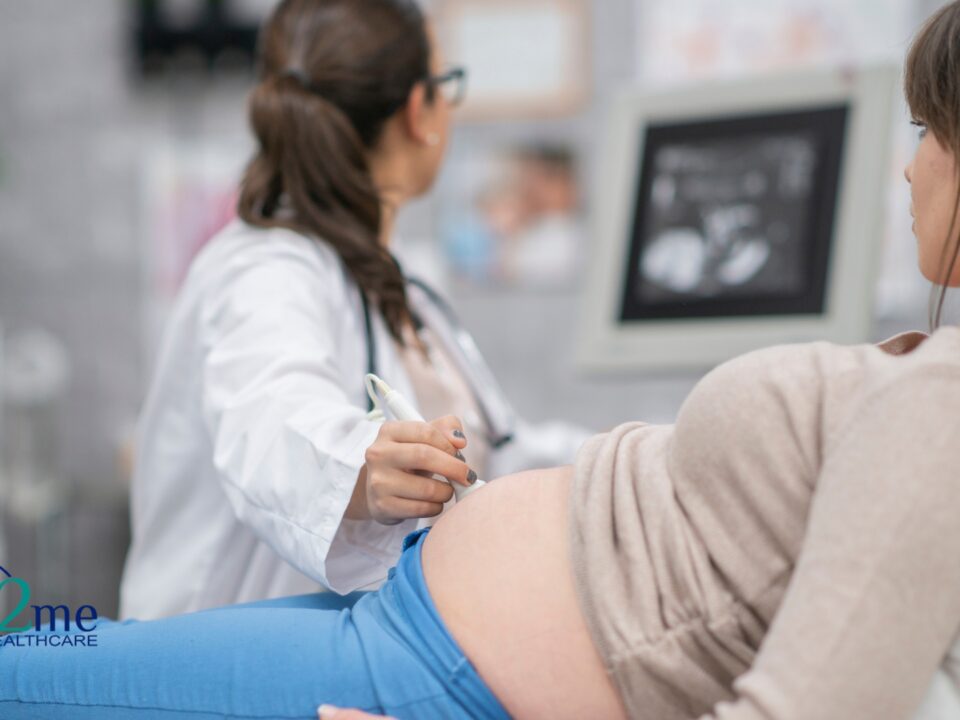
Diagnosis and the Power of Ultrasound
In decades past, VCI was often only discovered after birth when doctors examined the placenta. Today, advances in medical imaging allow for prenatal diagnosis.
VCI is typically identified during the 20-week anatomy scan. If your healthcare provider identifies a VCI, they will also perform a targeted scan to rule out vasa previa. Knowing the location of those vessels is the single most important factor in ensuring a safe delivery.
Managing a VCI Pregnancy
A VCI diagnosis often classifies a pregnancy as high-risk, ensuring a more proactive medical approach. Management focuses on rigorous monitoring and scans, and patients typically receive serial ultrasounds every 3–4 weeks to track fetal growth and non-stress tests (NST) to monitor the heart rate for signs of vessel compression.
Delivery planning depends on the presence of vasa previa. If VCI is isolated, vaginal delivery is often possible with continuous electronic fetal monitoring. However, if vasa previa is present, a planned C-section, usually between 34 and 36 weeks, is required to prevent vessel rupture during labor.
Navigating VCI With OB2Me
A VCI diagnosis requires vigilant monitoring, which can feel overwhelming in a traditional clinic setting. OB2Me transforms this experience by bringing specialized, high-touch prenatal care directly to you. Our concierge model offers in-home non-stress tests (NSTs) and personalized monitoring, reducing the stress of frequent office visits while ensuring fetal safety.
With 24/7 direct provider access and a focus on hospital-based delivery, OB2Me provides the expert oversight and peace of mind necessary for high-risk cord conditions. Empower your pregnancy journey with the support and convenience you deserve at OB2Me.